Medimaps Group presents data showing how new AI approach enhances osteoporosis diagnosis and monitoring at ECR 2023
Medimaps Group, presented data showing that its new spine segmentation (SpS) deep learning algorithm may be a reliable, time-efficient tool to enhance patient monitoring and osteoporosis diagnosis.
The results were obtained from a study using Medimaps Group’s SpS deep learning algorithm on thousands of scans from the OsteoLaus cohort and evaluated on an independent test set.
Read the abstract
Evaluation of a deep learning spine segmentation (SpS) algorithm for accurate and reproducible monitoring of lumbar spine DXA scans.
G Gatineau1, E H Ahmed2, K Hind 2, O Lamy1, E Gonzalez Rodriguez1, L Beaugé2,D Hans1,2
1Center of Bone Diseases, Rheumatology Unit, Bone and Joint Department, Lausanne University Hospital, & University of Lausanne, Lausanne, Switzerland 2Medimaps group SA, Plan-les-Ouates, Switzerland;
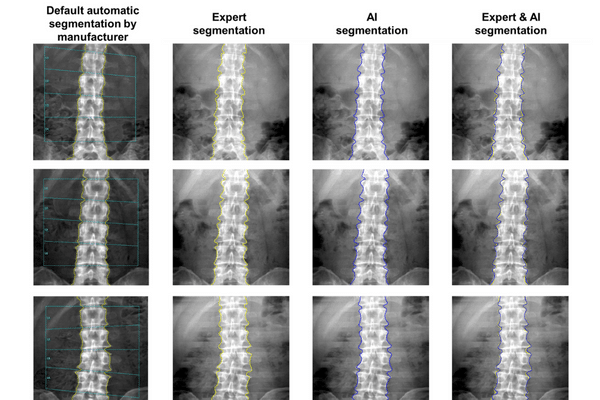
Purpose: The antero-posterior (AP) lumbar spine dual energy X-ray absorptiometry (DXA) scan is an important diagnostic measure, used for the assessment of osteoporosis. However, reducing technical error requires manual validation of the default spine segmentation (SpS) which can be time-consuming in practice. The aim of this study was to evaluate a new deep-learning artificial intelligence (AI) -based model for automated SpS.
Methods: A sub-sample of 130 women (age: 67.1; BMI: 25.2; no vertebral anomalies) were selected from the OsteoLaus cohort, having previously received two LS DXA (GE Lunar iDXA, encore v 18) 2.5 years apart. Scans were analyzed using the default, clinical expert and AI method to derive bone mineral density (BMD), trabecular bone score (TBS) and surface area). The coefficient of variation (CV%) for reproducibility of bone surface area was also computed.
Results: There were significant differences in bone outcomes between the default method and expert, but not between the AI SpS and expert (Table 1). Reproducibility for surface area was superior for the clinical expert and the AI model compared to the default (Table 2).
Table 1: Comparison of bone mineral density (BMD) and trabecular bone score (TBS) between three spine segmentation methods: default, clinical expert and deep learning AI-model
| Mean (SD) | Mean (SD) | Mean (SD) | Mean (SD) | Mean (SD) | p-value |
| L1L4 BMD | Expert | 1.003 (0.156) | AI | 1.006 (0.158) | 0.67 |
| L1L4 BMD | Expert | 1.003 (0.156) | Default | 1.034 (0.145) | 0.01* |
| L1L4 TBS | Expert | 1.326 (0.084) | AI | 1.325 (0.084) | 0.84 |
| L1L4 TBS | Expert | 1.326 (0.084) | Default | 1.296 (0.091) | < 0.001* |
Table 2: Bone surface area reproducibility (CV%) for the default, clinical expert and deep learning AI model
| A | B | Mean (SD) | Mean 2 (SD) | p-value | |
| L1L4 surface CV% | Default | AI | 1.61 (1.56) | 0.932 (0.685) | < 0.001* |
| L1L4 surface CV% | Expert | Default | 0.985 (0.898) | 1.61 (1.56) | < 0.001* |
| L1L4 surface CV% | Expert | AI | 0.985 (0.898) | 0.932 (0.685) | 0.496 |
Conclusion: The new deep learning AI based model demonstrated improved accuracy and reproducibility for lumbar spine bone segmentation compared to the default, and in close agreement with the clinical expert. Overall, these results suggest that the new AI-based model for automated SpS may be a valuable, time-efficient tool for the analysis of lumbar spine DXA scans.
Limitations: Future work should validate the model in larger, diverse cohorts and with different DXA systems